20 results
Subsurface scientific exploration of extraterrestrial environments (MINAR 5): analogue science, technology and education in the Boulby Mine, UK – CORRIGENDUM
- Charles S. Cockell, John Holt, Jim Campbell, Harrison Groseman, Jean-Luc Josset, Tomaso R. R. Bontognali, Audra Phelps, Lilit Hakobyan, Libby Kuretn, Annalea Beattie, Jen Blank, Rosalba Bonaccorsi, Christopher McKay, Anushree Shirvastava, Carol Stoker, David Willson, Scott McLaughlin, Sam Payler, Adam Stevens, Jennifer Wadsworth, Loredana Bessone, Matthias Maurer, Francesco Sauro, Javier Martin-Torres, Maria-Paz Zorzano, Anshuman Bhardwaj, Alvaro Soria-Salinas, Thasshwin Mathanlal, Miracle Israel Nazarious, Abhilash Vakkada Ramachandran, Parag Vaishampayan, Lisa Guan, Scott M. Perl, Jon Telling, Ian M. Boothroyd, Ollie Tyson, James Realff, Joseph Rowbottom, Boris Laurent, Matt Gunn, Shaily Shah, Srijan Singh, Sean Paling, Tom Edwards, Louise Yeoman, Emma Meehan, Christopher Toth, Paul Scovell, Barbara Suckling
-
- Journal:
- International Journal of Astrobiology / Volume 23 / 2024
- Published online by Cambridge University Press:
- 06 November 2023, e2
-
- Article
-
- You have access Access
- HTML
- Export citation
Identifying the relationship between hospital rurality and antibiotic overuse
- Hannah Hardin, Valerie Vaughn, Andrea White, Jennifer Horowitz, Elizabeth McLaughlin, Julia Szymczak, Lindsay Petty, Anurag Malani, Scott Flanders, Tejal Gandhi
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s34-s35
-
- Article
-
- You have access Access
- Open access
- Export citation
-
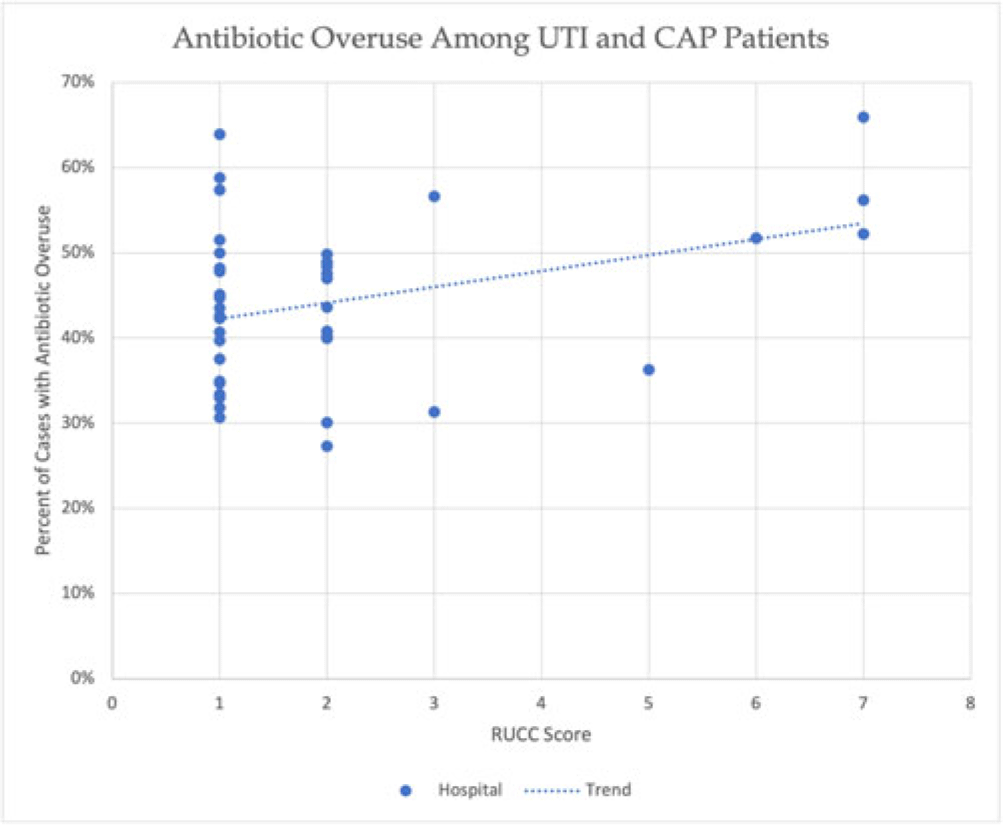
Background: Antibiotic overuse and the resulting patient outcomes span all hospitals. However, although antibiotic stewardship can improve antibiotic use, effective stewardship programs require expertise and an infrastructure that are not present in all hospitals. Rural hospitals have less access to resources, infectious disease expertise, and participation in academic research. Thus, we compared antibiotic overuse at discharge between rural and nonrural hospitals for patients diagnosed with community-associated pneumonia (CAP) or urinary tract infection (UTI)—the 2 most common hospital infections. Methods: To determine whether antibiotic overuse at discharge was higher among rural versus nonrural hospitals, we analyzed data from a 41-hospital prospective cohort of patients treated for CAP or UTI between July 1, 2017, and July 30, 2019, in Michigan. Antibiotic overuse was defined as treatment that was unnecessary (ie, patient did not have an infection), excessive (ie, duration >4 days for CAP), or included suboptimal fluoroquinolone use (ie, safer alternative available). Overuse was determined based on patient risk factors, symptoms, allergies, diagnostic results, and time to stability. Hospital rurality was defined using the Rural–Urban Continuum Codes (RUCC) score. We defined rural as a score ≥4 and very rural as a score of 7–9. We used t tests to compare the mean percentage of patients with antibiotic overuse at discharge between nonrural and rural (and very rural) hospitals. Results: Across 41 hospitals, we included 23,449 patients with CAP or UTI. There were 5 rural (and 3 very rural) hospitals with 2,039 (and 1,082) patients. Antibiotic overuse at discharge was present in 43.1% of patient cases in nonrural hospitals, 52.5% in rural hospitals (P = .04 vs nonrural) and 58.1% in very rural hospitals (P = .007 vs nonrural). Compared to nonrural hospitals, the mean percentage of cases with antibiotic overuse at discharge in rural hospitals was 9.4% higher (15.1% higher in very rural hospitals). Results were similar in a subgroup analysis of only patients with UTI (47.0% in rural vs 37.5% in nonrural, mean difference, 9.5%; P = .03) but were not statistically significant in patients with CAP (53.8% vs 48.0%, respectively; mean difference, 5.8%; P = 0.23). Conclusions: In this retrospective study, rural hospitals—especially very rural hospitals, had higher rates of antibiotic overuse at discharge than nonrural hospitals. Our findings suggest that antibiotic stewardship interventions tailored toward the unique differences in infrastructure, resources, and needs of rural hospitals are essential to community health.
Disclosures: None
Three-day antibiotic duration in patients with pneumonia: A sixty-eight–hospital cohort
- Valerie Vaughn, Lindsay Petty, David Ratz, Elizabeth McLaughlin, Tawny Czilok, Jennifer Horowitz, Anurag Malani, Danielle Osterholzer, Scott Flanders, Tejal Gandhi
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s22
-
- Article
-
- You have access Access
- Open access
- Export citation
-
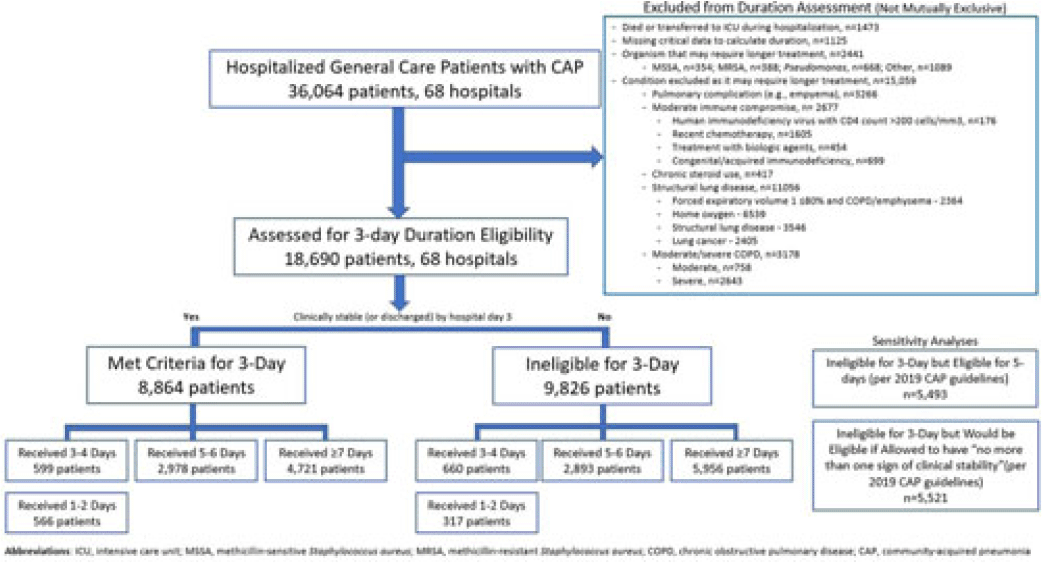
Background: Since 2019, community-acquired pneumonia (CAP) guidelines have recommended hospitalized patients be treated until clinical “stability and for no less than 5 days.” However, randomized trials have reported that, in patients who stabilize by hospital day 3, very short antibiotic durations (eg, 3 days) are noninferior to longer durations. How these trial results relate to real-world practice is unknown. Methods: Using a 68-hospital cohort study of hospitalized, general-care adults with CAP, we aimed to (1) quantify the percentage of patients who—according to trial criteria—qualify for a 3-day antibiotic duration, (2) quantify the percentage who actually received a 3-day duration, and (3) assess 30-day outcomes. Patients were considered to have CAP if they had a pneumonia discharge diagnosis and met clinical criteria for CAP. Patients with concomitant infections (including COVID-19), admission to intensive care, or severe immunocompromise were not included. Results: Between February 23, 2017, and August 3, 2022, 36,064 patients with CAP were included. Of those, 48.2% (9,826 of 36,064) were excluded due to a condition or organism ineligible for the 3-day treatment (Fig. 1). Of the 18,690 patients remaining, 52.6% (9,826) were unstable on day 3 and thus were ineligible for the 3-day treatment. Therefore, of all 36,064 patients, only 8,864 (24.6%) would be eligible under trial criteria for a 3-day treatment. Notably, 5,493 (55.9%) of 9,826 patients unstable on day 3 would be eligible for 5 days of treatment under national guidelines. In practice, use of 3–4-day treatment was rare, occurring in 599 (6.8%) of 8,864 patients eligible for a 3-day treatment versus 660 (6.7%) of 9,826 patients unstable on day 3 (P = .945). Use of 3–4-day treatment increased over time and comorbidities that could mimic CAP or a negative procalcitonin were more common in patients who received a 3–4-day treatment whereas specific symptoms of CAP were less common (Fig. 2). After adjustments, patients eligible for a 3-day duration who received a 3–4 day treatment versus a ≥5-day treatment had higher 30-day mortality (aOR, 1.87; 95% CI, 1.32–2.64) and readmission (aOR, 1.35; 95% CI, 1.17–1.56). Conclusions: Across 68 hospitals, <25% of patients hospitalized with CAP would be eligible for a 3-day antibiotic treatment. Though increasing over time, there was little use of 3–4-day treatments and, when prescribed, outcomes were worse, potentially due to CAP misdiagnosis. Given the small number of patients eligible for 3-day treatment, and the potential harm with too-short durations, it may be prudent to focus on increasing the use of 5-day treatments.
Disclosures: None
Risk Factors and outcomes associated with inappropriate empiric broad-spectrum antibiotic use in hospitalized patients with community-acquired pneumonia
- Tejal Gandhi, Lindsay Petty, Valerie Vaughn, Anurag Malani, David Ratz, Tawny Czilok, Jennifer Horowitz, Elizabeth McLaughlin, Lisa Dumkow, Stephanie Burdick, Danielle Osterholzer, Mariam Younas, Steven Bernstein, Scott Flanders
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s31-s32
-
- Article
-
- You have access Access
- Open access
- Export citation
-
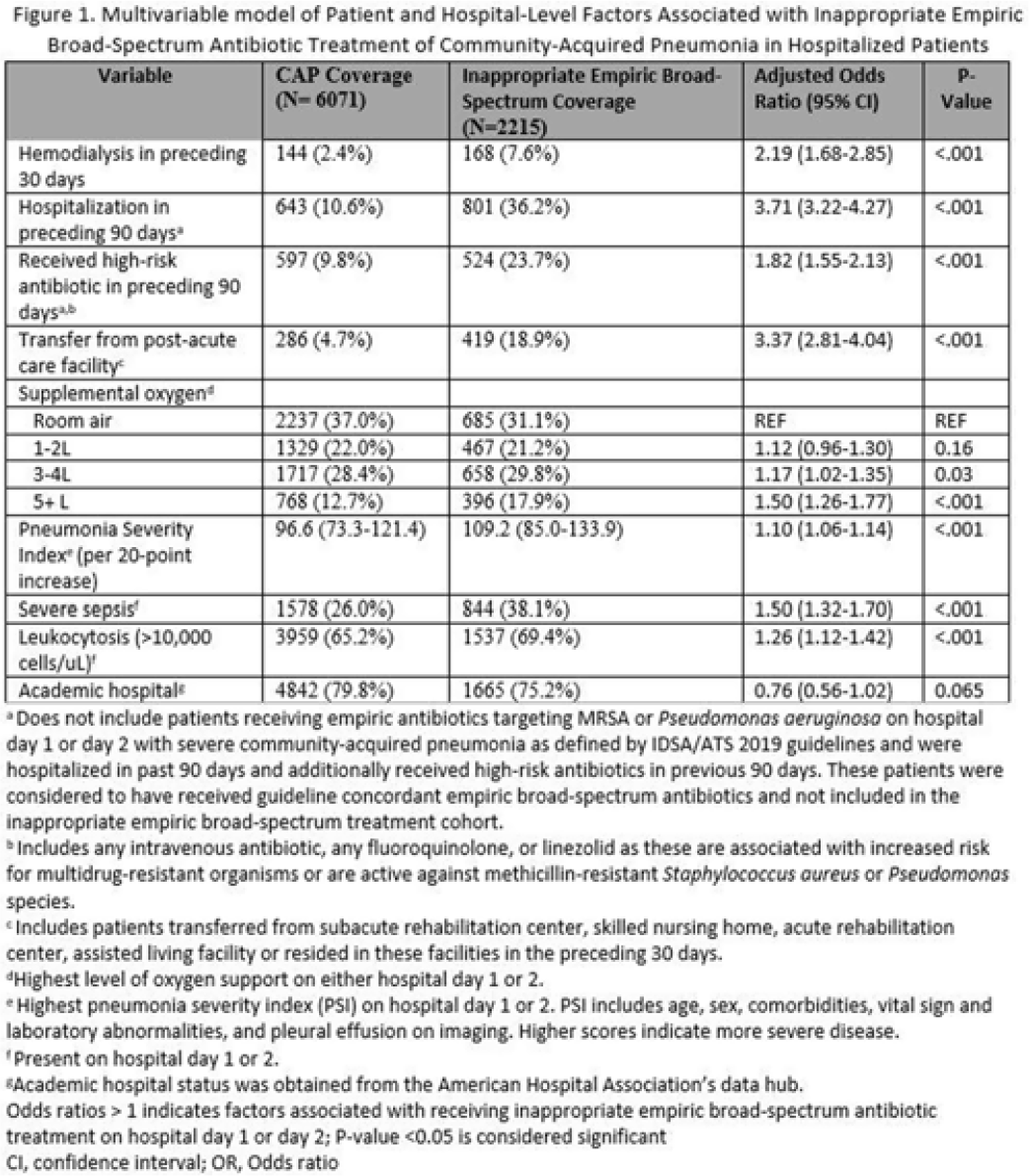
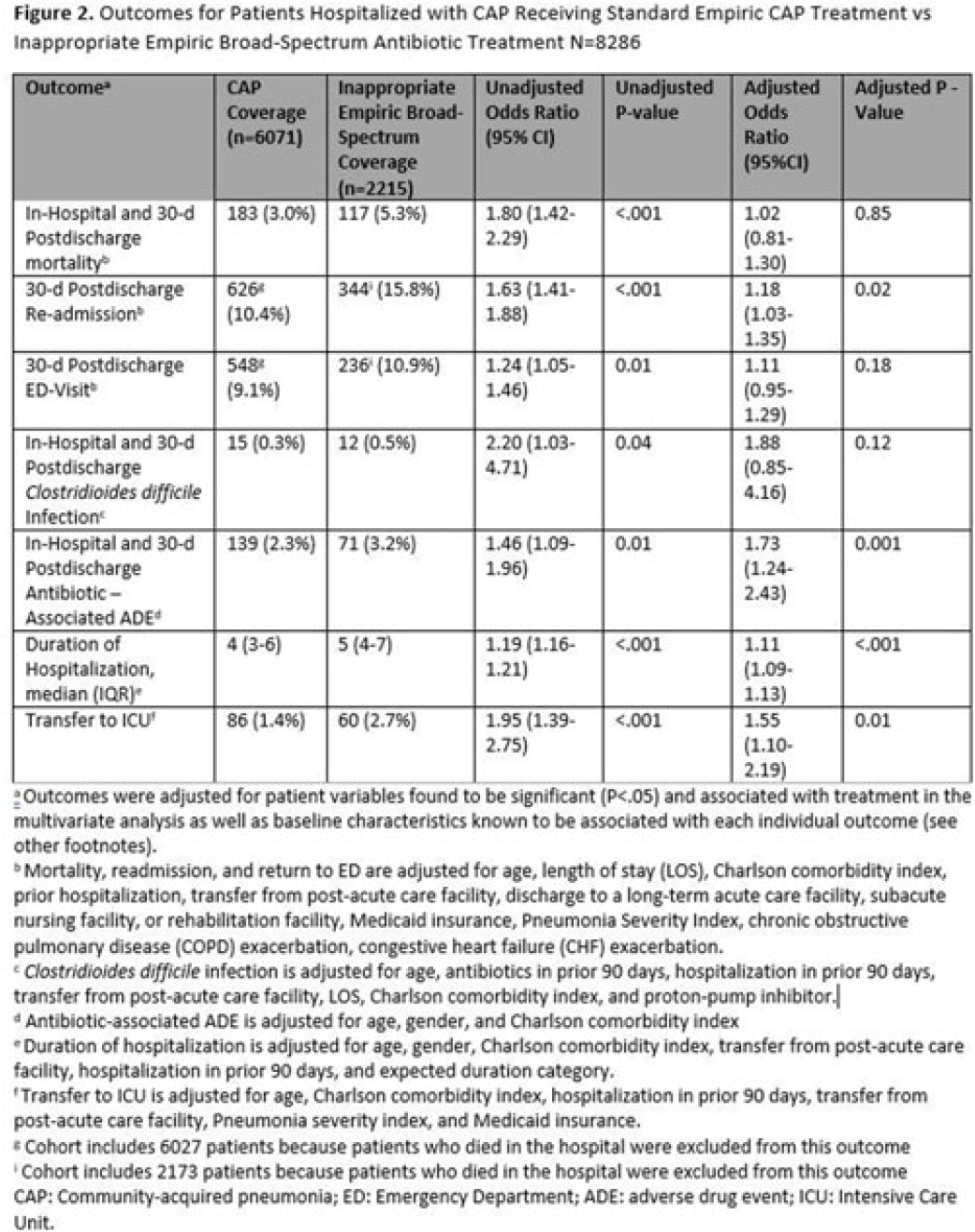
Background: Inappropriate broad-spectrum antibiotic use targeting methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa can result in increased adverse events, antibiotic resistance, and Clostridioides difficile infection. In 2019, revised ATS/IDSA community-acquired pneumonia (CAP) guidelines removed healthcare-associated pneumonia (HCAP) as a clinical entity and modified patient factors warranting empiric broad-spectrum antibiotic (BSA) use. As a result, most patients hospitalized with CAP should receive empiric antibiotics targeting standard CAP pathogens. Based on revised guidelines, we evaluated predictors and outcomes associated with inappropriate BSA use among hospitalized patients with CAP. Methods: Between November 2019 and July 2022, trained abstractors collected data on non-ICU adult medical patients admitted with CAP at 67 Michigan hospitals who received either an inappropriate empiric BSA on hospital day 1 or 2 or a standard CAP regimen. Inappropriate empiric BSA use was defined as use of an anti-MRSA or anti-pseudomonal antibiotic in a patient eligible for standard CAP coverage per IDSA guidelines. Patients with immune compromise, moderate or severe chronic obstructive pulmonary disease (COPD), pulmonary complication, or guideline-concordant treatment with BSA were excluded. Data collected included comorbidities, antibiotic use and hospitalizations in the preceding 90 days, cultures in the preceding year, signs or symptoms of pneumonia, hospital characteristics, and 30-day postdischarge patient outcomes. Data were collected through chart review and patient phone calls. Predictors of inappropriate empiric BSA were evaluated using logistic general estimating equation (GEE) models, accounting for hospital-level clustering. We assessed the effect of inappropriate empiric BSA (vs standard CAP therapy) on 30-day patient outcomes using logistic GEE models controlling for predictors associated with the outcome and probability of treatment. Results: Of 8,286 included patients with CAP, 2,215 (26.7%) were empirically treated with inappropriate BSA. The median BSA treatment was 3 days (IQR, 2.5). After adjustments, factors associated with inappropriate empiric BSA treatment included hospitalization or treatment with high-risk antibiotics in preceding 90 days, transfer from a postacute care facility, hemodialysis, support with ≥3 L supplemental oxygen, severe sepsis, leukocytosis, and higher pneumonia severity index (Fig. 1). After adjustments, patients with inappropriate empiric BSA treatment had higher readmissions 30 days after discharge, more transfers to the intensive care unit, more antibiotic-associated adverse events, and longer hospitalizations (Fig. 2). Conclusions: Patients hospitalized with CAP often received inappropriate BSA as empiric coverage, and this inappropriate antibiotic selection was associated with worse patient outcomes. To improve patient outcomes, stewardship efforts should focus on reducing inappropriate BSA use in patients hospitalized for CAP with historic HCAP risk factors or severe CAP without other guideline-directed indications for BSA.
Financial support. H.M.S. initiative is underwritten by Blue Cross and Blue Shield of Michigan.
Disclosures: None
TEACHING COMPOSITION IN A FLIPPED CLASSROOM
- Martin Iddon, Scott McLaughlin
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
In 2019 the present authors, along with our colleague Mic Spencer, began work on a project funded by the Leeds Institute for Teaching Excellence, designed to look at the ways in which we taught composition at the University of Leeds and how we might change them. Mic has focused on postgraduate teaching, and we have considered the earliest parts of the undergraduate curriculum, particularly the first two years of study, when the largest numbers of students with the least experience of the study of composition at tertiary level might be in a classroom (50 or so, in our case).
Risk factors and outcomes associated with community-onset and hospital-acquired coinfection in patients hospitalized for coronavirus disease 2019 (COVID-19): A multihospital cohort study
- Part of
- Lindsay A. Petty, Scott A. Flanders, Valerie M. Vaughn, David Ratz, Megan O’Malley, Anurag N. Malani, Laraine Washer, Tae Kim, Keith E. Kocher, Scott Kaatz, Tawny Czilok, Elizabeth McLaughlin, Hallie C. Prescott, Vineet Chopra, Tejal Gandhi
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 9 / September 2022
- Published online by Cambridge University Press:
- 26 July 2021, pp. 1184-1193
- Print publication:
- September 2022
-
- Article
- Export citation
-
Background:
We sought to determine the incidence of community-onset and hospital-acquired coinfection in patients hospitalized with coronavirus disease 2019 (COVID-19) and to evaluate associated predictors and outcomes.
Methods:In this multicenter retrospective cohort study of patients hospitalized for COVID-19 from March 2020 to August 2020 across 38 Michigan hospitals, we assessed prevalence, predictors, and outcomes of community-onset and hospital-acquired coinfections. In-hospital and 60-day mortality, readmission, discharge to long-term care facility (LTCF), and mechanical ventilation duration were assessed for patients with versus without coinfection.
Results:Of 2,205 patients with COVID-19, 141 (6.4%) had a coinfection: 3.0% community onset and 3.4% hospital acquired. Of patients without coinfection, 64.9% received antibiotics. Community-onset coinfection predictors included admission from an LTCF (OR, 3.98; 95% CI, 2.34–6.76; P < .001) and admission to intensive care (OR, 4.34; 95% CI, 2.87–6.55; P < .001). Hospital-acquired coinfection predictors included fever (OR, 2.46; 95% CI, 1.15–5.27; P = .02) and advanced respiratory support (OR, 40.72; 95% CI, 13.49–122.93; P < .001). Patients with (vs without) community-onset coinfection had longer mechanical ventilation (OR, 3.31; 95% CI, 1.67–6.56; P = .001) and higher in-hospital mortality (OR, 1.90; 95% CI, 1.06–3.40; P = .03) and 60-day mortality (OR, 1.86; 95% CI, 1.05–3.29; P = .03). Patients with (vs without) hospital-acquired coinfection had higher discharge to LTCF (OR, 8.48; 95% CI, 3.30–21.76; P < .001), in-hospital mortality (OR, 4.17; 95% CI, 2.37–7.33; P ≤ .001), and 60-day mortality (OR, 3.66; 95% CI, 2.11–6.33; P ≤ .001).
Conclusion:Despite community-onset and hospital-acquired coinfection being uncommon, most patients hospitalized with COVID-19 received antibiotics. Admission from LTCF and to ICU were associated with increased risk of community-onset coinfection. Future studies should prospectively validate predictors of COVID-19 coinfection to facilitate the reduction of antibiotic use.
Antibiotic Overuse at Discharge in Hospitalized Patients with Bacteriuria or Treated for Pneumonia: A Multihospital Study
- Valerie M Vaughn, Lindsay A. Petty, Tejal N. Gandhi, Keith S. Kaye, Anurag Malani, Steven J. Bernstein, David Ratz, Elizabeth McLaughlin, Scott A. Flanders
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s459-s461
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Nearly half of hospitalized patients with bacteriuria or treated for pneumonia receive unnecessary antibiotics (noninfectious or nonbacterial syndrome such as asymptomatic bacteriuria), excess duration (antibiotics prescribed for longer than necessary), or avoidable fluoroquinolones (safer alternative available) at hospital discharge.1–3 However, whether antibiotic overuse at discharge varies between hospitals or is associated with patient outcomes remains unknown. Methods: From July 2017 to December 2018, trained abstractors at 46 Michigan hospitals collected detailed data on a sample of adult, non–intensive care, hospitalized patients with bacteriuria (positive urine culture with or without symptoms) or treated for community-acquired pneumonia (CAP; includes those with the disease formerly known as healthcare-associated pneumonia [HCAP]). Antibiotic prescriptions at discharge were assessed for antibiotic overuse using a previously described, guideline-based hierarchical algorithm.3 Here, we report the proportion of patients discharged with antibiotic overuse by the hospital. We also assessed hospital-level correlation (using Pearson’s correlation coefficient) between antibiotic overuse at discharge for patients with bacteriuria and patients treated for CAP. Finally, we assessed the association of antibiotic overuse at discharge with patient outcomes (mortality, readmission, emergency department visit, and antibiotic-associated adverse events) at 30 days using logit generalized estimating equations adjusted for patient characteristics and probability of treatment. Results: Of 17,081 patients (7,207 with bacteriuria; 9,874 treated for pneumonia), nearly half (42.2%) had antibiotic overuse at discharge (36.3% bacteriuria and 51.1% pneumonia). The percentage of patients discharged with antibiotic overuse varied 5-fold among hospitals from 14.7% (95% CI, 8.0%–25.3%) to 74.3% (95% CI, 64.2%–83.8%). Hospital rates of antibiotic overuse at discharge were strongly correlated between bacteriuria and CAP (Pearson’s correlation coefficient, 0.76; P ≤ .001) (Fig. 1). In adjusted analyses, antibiotic overuse at discharge was not associated with death, readmission, emergency department visit, or Clostridioides difficile infection. However, each day of overuse was associated with a 5% increase in the odds of patient-reported antibiotic-associated adverse events after discharge (Fig. 2). Conclusions: Antibiotic overuse at discharge was common, varied widely between hospitals, and was associated with patient harm. Furthermore, antibiotic overuse at discharge was strongly correlated between 2 disparate diseases, suggesting that prescribing culture or discharge processes—rather than disease-specific factors—contribute to overprescribing at discharge. Thus, discharge stewardship may be needed to target multiple diseases.
Funding: This study was supported by the Society for Healthcare Epidemiology of America and by Blue Cross Blue Shield of Michigan and Blue Care Network.
Disclosures: Valerie M. Vaughn reports contracted research for Blue Cross and Blue Shield of Michigan, the Department of VA, the NIH, the SHEA, and the APIC. She also reports receipt of funds from the Gordon and Betty Moore Foundation Speaker’s Bureau, the CDC, the Pew Research Trust, Sepsis Alliance, and the Hospital and Health System Association of Pennsylvania.
Misdiagnosis of Urinary Tract Infection Linked to Misdiagnosis of Pneumonia: A Multihospital Cohort Study
- Valerie M. Vaughn, Ashwin Gupta, Lindsay A. Petty, Tejal N. Gandhi, Scott A. Flanders, Lakshmi Swaminathan, Lama Hsaiky, Lama Hsaiky, David Ratz, Jennifer Horowitz, Elizabeth McLaughlin, Vineet Chopra
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s488-s489
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Clinicians often diagnose bacterial infections such as urinary tract infection (UTI) and pneumonia in patients who are asymptomatic or have nonbacterial causes of their symptoms. Misdiagnosis of infection leads to unnecessary antibiotic use and potentially delays correct diagnoses. Interventions to improve diagnosis often focus on infections separately. However, if misdiagnosis is linked, broader interventions to improve diagnosis may be more effective. Thus, we assessed whether misdiagnosis of UTI and community-acquired pneumonia (CAP) was correlated. Methods: From July 2017 to July 2019, abstractors at 46 Michigan hospitals collected data on a sample of adult, non–intensive care, hospitalized patients with bacteriuria (positive urine culture) or who were treated for presumed CAP (discharge diagnosis plus antibiotics). Patients with concomitant bacterial infections were excluded. Using a previously described method,1,2 patients were assessed for UTI or CAP based on symptoms, signs, and laboratory or radiology findings. Misdiagnosis of UTI was defined as patients with asymptomatic bacteriuria (ASB) treated with antibiotics number of patients with bacteriuria Misdiagnosis of CAP was defined as patients treated for presumed CAP who did not have CAP number of patients treated for presumed CAP. Hospital-level correlation was assessed using Pearson’s correlation coefficient between misdiagnosis of UTI and CAP. For patients with prescriber data (N = 3,293), we also assessed emergency department (ED)-level correlation. Results: Of 11,914 patients with bacteriuria, 31.9% (N = 3,796) had ASB. Of those, 2,973 of 3,796 (78.3%) received antibiotics. Of 14,085 patients treated for CAP, 1,602 (11.4%) did not have CAP. Incidence of misdiagnosis varied by hospital: those with high rates of misdiagnosis of UTI were more likely to have high rates of misdiagnosis of CAP (Pearson’s correlation coefficient, 0.58; P ≤ .001) (Fig. 1). Of 2,137 patients misdiagnosed with UTI, 1,159 (54.2%) had antibiotic treatment started in the ED; of those, 942 (81.3%) remained on antibiotics on day 3 of hospitalization. Of 1,156 patients misdiagnosed with CAP, 871 (75.3%) had antibiotic therapy started in the ED, and 789 of these 871 patients (90.6%) were still on antibiotics on day 3 of hospitalization. Hospitals with high rates of UTI misdiagnosis in the ED were more likely to have high rates of CAP misdiagnosis in the ED (Pearson’s correlation coefficient, 0.33; P ≤ .001). Conclusions: Misdiagnosis of 2 unrelated infections was moderately correlated by hospital and weakly correlated by hospital ED. Potential causes include differences in organizational culture (eg, low tolerance for diagnostic uncertainty, emergency department culture), organizational initiatives (eg, sepsis, stewardship), or coordination between emergency and hospital medicine. Additionally, antibiotics initiated in the ED were typically continued following admission, potentially reflecting diagnosis momentum.
Funding: This work was supported by Blue Cross Blue Shield of Michigan and Blue Care Network.
Disclosures: Valerie M. Vaughn reports contract research for Blue Cross and Blue Shield of Michigan, the Department of Veterans’ Affairs, the NIH, the SHEA, and the APIC. She also reports fees from the Gordon and Betty Moore Foundation Speaker’s Bureau, the CDC, the Pew Research Trust, Sepsis Alliance, and The Hospital and Health System Association of Pennsylvania.
Chapter 17 - DSM-5 and ICD-11 Definitions of Posttraumatic Stress Disorder: Investigating “Narrow” and “Broad” Approaches
- from Section 5 - Dissecting the Clinical Picture
- Edited by Evelyn J. Bromet, State University of New York, Stony Brook, Elie G. Karam, Karestan C. Koenen, Harvard University, Massachusetts, Dan J. Stein, University of Cape Town
-
- Book:
- Trauma and Posttraumatic Stress Disorder
- Published online:
- 26 July 2018
- Print publication:
- 09 August 2018, pp 253-262
-
- Chapter
- Export citation
Subsurface scientific exploration of extraterrestrial environments (MINAR 5): analogue science, technology and education in the Boulby Mine, UK
- Charles S. Cockell, John Holt, Jim Campbell, Harrison Groseman, Jean-Luc Josset, Tomaso R. R. Bontognali, Audra Phelps, Lilit Hakobyan, Libby Kuretn, Annalea Beattie, Jen Blank, Rosalba Bonaccorsi, Christopher McKay, Anushree Shirvastava, Carol Stoker, David Willson, Scott McLaughlin, Sam Payler, Adam Stevens, Jennifer Wadsworth, Loredana Bessone, Matthias Maurer, Francesco Sauro, Javier Martin-Torres, Maria-Paz Zorzano, Anshuman Bhardwaj, Alvaro Soria-Salinas, Thasshwin Mathanlal, Miracle Israel Nazarious, Abhilash Vakkada Ramachandran, Parag Vaishampayan, Lisa Guan, Scott M. Perl, Jon Telling, Ian M. Boothroyd, Ollie Tyson, James Realff, Joseph Rowbottom, Boris Laurent, Matt Gunn, Shaily Shah, Srijan Singh, Sean Paling, Tom Edwards, Louise Yeoman, Emma Meehan, Christopher Toth, Paul Scovell, Barbara Suckling
-
- Journal:
- International Journal of Astrobiology / Volume 18 / Issue 2 / April 2019
- Published online by Cambridge University Press:
- 02 July 2018, pp. 157-182
-
- Article
- Export citation
-
The deep subsurface of other planetary bodies is of special interest for robotic and human exploration. The subsurface provides access to planetary interior processes, thus yielding insights into planetary formation and evolution. On Mars, the subsurface might harbour the most habitable conditions. In the context of human exploration, the subsurface can provide refugia for habitation from extreme surface conditions. We describe the fifth Mine Analogue Research (MINAR 5) programme at 1 km depth in the Boulby Mine, UK in collaboration with Spaceward Bound NASA and the Kalam Centre, India, to test instruments and methods for the robotic and human exploration of deep environments on the Moon and Mars. The geological context in Permian evaporites provides an analogue to evaporitic materials on other planetary bodies such as Mars. A wide range of sample acquisition instruments (NASA drills, Small Planetary Impulse Tool (SPLIT) robotic hammer, universal sampling bags), analytical instruments (Raman spectroscopy, Close-Up Imager, Minion DNA sequencing technology, methane stable isotope analysis, biomolecule and metabolic life detection instruments) and environmental monitoring equipment (passive air particle sampler, particle detectors and environmental monitoring equipment) was deployed in an integrated campaign. Investigations included studying the geochemical signatures of chloride and sulphate evaporitic minerals, testing methods for life detection and planetary protection around human-tended operations, and investigations on the radiation environment of the deep subsurface. The MINAR analogue activity occurs in an active mine, showing how the development of space exploration technology can be used to contribute to addressing immediate Earth-based challenges. During the campaign, in collaboration with European Space Agency (ESA), MINAR was used for astronaut familiarization with future exploration tools and techniques. The campaign was used to develop primary and secondary school and primary to secondary transition curriculum materials on-site during the campaign which was focused on a classroom extra vehicular activity simulation.
Trauma and psychotic experiences: transnational data from the World Mental Health Survey
- John J. McGrath, Sukanta Saha, Carmen C. W. Lim, Sergio Aguilar-Gaxiola, Jordi Alonso, Laura H. Andrade, Evelyn J. Bromet, Ronny Bruffaerts, José M. Caldas de Almeida, Graça Cardoso, Giovanni de Girolamo, John Fayyad, Silvia Florescu, Oye Gureje, Josep M. Haro, Norito Kawakami, Karestan C. Koenen, Viviane Kovess-Masfety, Sing Lee, Jean-Pierre Lepine, Katie A. McLaughlin, Maria E. Medina-Mora, Fernando Navarro-Mateu, Akin Ojagbemi, Jose Posada-Villa, Nancy Sampson, Kate M. Scott, Hisateru Tachimori, Margreet ten Have, Kenneth S. Kendler, Ronald C. Kessler,
-
- Journal:
- The British Journal of Psychiatry / Volume 211 / Issue 6 / December 2017
- Published online by Cambridge University Press:
- 02 January 2018, pp. 373-380
- Print publication:
- December 2017
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
Traumatic events are associated with increased risk of psychotic experiences, but it is unclear whether this association is explained by mental disorders prior to psychotic experience onset.
AimsTo investigate the associations between traumatic events and subsequent psychotic experience onset after adjusting for post-traumatic stress disorder and other mental disorders.
MethodWe assessed 29 traumatic event types and psychotic experiences from the World Mental Health surveys and examined the associations of traumatic events with subsequent psychotic experience onset with and without adjustments for mental disorders.
ResultsRespondents with any traumatic events had three times the odds of other respondents of subsequently developing psychotic experiences (OR=3.1, 95% CI 2.7–3.7), with variability in strength of association across traumatic event types. These associations persisted after adjustment for mental disorders.
ConclusionsExposure to traumatic events predicts subsequent onset of psychotic experiences even after adjusting for comorbid mental disorders.
X-Ray and Optical Properties of Black Widows and Redbacks
- Mallory S.E. Roberts, Hind Al Noori, Rodrigo A. Torres, Maura A. McLaughlin, Peter A. Gentile, Jason W.T. Hessels, Scott M. Ransom, Paul S. Ray, Matthew Kerr, Rene P. Breton
-
- Journal:
- Proceedings of the International Astronomical Union / Volume 13 / Issue S337 / September 2017
- Published online by Cambridge University Press:
- 04 June 2018, pp. 43-46
- Print publication:
- September 2017
-
- Article
-
- You have access Access
- Export citation
-
Black widows and redbacks are binary systems consisting of a millisecond pulsar in a close binary with a companion having matter driven off of its surface by the pulsar wind. X-rays due to an intrabinary shock have been observed from many of these systems, as well as orbital variations in the optical emission from the companion due to heating and tidal distortion. We have been systematically studying these systems in radio, optical and X-rays. Here we will present an overview of X-ray and optical studies of these systems, including new XMM-Newton and NuStar data obtained from several of them, along with new optical photometry.
Posttraumatic stress disorder in the World Mental Health Surveys
- K. C. Koenen, A. Ratanatharathorn, L. Ng, K. A. McLaughlin, E. J. Bromet, D. J. Stein, E. G. Karam, A. Meron Ruscio, C. Benjet, K. Scott, L. Atwoli, M. Petukhova, C. C.W. Lim, S. Aguilar-Gaxiola, A. Al-Hamzawi, J. Alonso, B. Bunting, M. Ciutan, G. de Girolamo, L. Degenhardt, O. Gureje, J. M. Haro, Y. Huang, N. Kawakami, S. Lee, F. Navarro-Mateu, B.-E. Pennell, M. Piazza, N. Sampson, M. ten Have, Y. Torres, M. C. Viana, D. Williams, M. Xavier, R. C. Kessler,
-
- Journal:
- Psychological Medicine / Volume 47 / Issue 13 / October 2017
- Published online by Cambridge University Press:
- 07 April 2017, pp. 2260-2274
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
Traumatic events are common globally; however, comprehensive population-based cross-national data on the epidemiology of posttraumatic stress disorder (PTSD), the paradigmatic trauma-related mental disorder, are lacking.
MethodsData were analyzed from 26 population surveys in the World Health Organization World Mental Health Surveys. A total of 71 083 respondents ages 18+ participated. The Composite International Diagnostic Interview assessed exposure to traumatic events as well as 30-day, 12-month, and lifetime PTSD. Respondents were also assessed for treatment in the 12 months preceding the survey. Age of onset distributions were examined by country income level. Associations of PTSD were examined with country income, world region, and respondent demographics.
ResultsThe cross-national lifetime prevalence of PTSD was 3.9% in the total sample and 5.6% among the trauma exposed. Half of respondents with PTSD reported persistent symptoms. Treatment seeking in high-income countries (53.5%) was roughly double that in low-lower middle income (22.8%) and upper-middle income (28.7%) countries. Social disadvantage, including younger age, female sex, being unmarried, being less educated, having lower household income, and being unemployed, was associated with increased risk of lifetime PTSD among the trauma exposed.
ConclusionsPTSD is prevalent cross-nationally, with half of all global cases being persistent. Only half of those with severe PTSD report receiving any treatment and only a minority receive specialty mental health care. Striking disparities in PTSD treatment exist by country income level. Increasing access to effective treatment, especially in low- and middle-income countries, remains critical for reducing the population burden of PTSD.
The epidemiology of traumatic event exposure worldwide: results from the World Mental Health Survey Consortium
- C. Benjet, E. Bromet, E. G. Karam, R. C. Kessler, K. A. McLaughlin, A. M. Ruscio, V. Shahly, D. J. Stein, M. Petukhova, E. Hill, J. Alonso, L. Atwoli, B. Bunting, R. Bruffaerts, J. M. Caldas-de-Almeida, G. de Girolamo, S. Florescu, O. Gureje, Y. Huang, J. P. Lepine, N. Kawakami, Viviane Kovess-Masfety, M. E. Medina-Mora, F. Navarro-Mateu, M. Piazza, J. Posada-Villa, K. M. Scott, A. Shalev, T. Slade, M. ten Have, Y. Torres, M. C. Viana, Z. Zarkov, K. C. Koenen
-
- Journal:
- Psychological Medicine / Volume 46 / Issue 2 / January 2016
- Published online by Cambridge University Press:
- 29 October 2015, pp. 327-343
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
Considerable research has documented that exposure to traumatic events has negative effects on physical and mental health. Much less research has examined the predictors of traumatic event exposure. Increased understanding of risk factors for exposure to traumatic events could be of considerable value in targeting preventive interventions and anticipating service needs.
MethodGeneral population surveys in 24 countries with a combined sample of 68 894 adult respondents across six continents assessed exposure to 29 traumatic event types. Differences in prevalence were examined with cross-tabulations. Exploratory factor analysis was conducted to determine whether traumatic event types clustered into interpretable factors. Survival analysis was carried out to examine associations of sociodemographic characteristics and prior traumatic events with subsequent exposure.
ResultsOver 70% of respondents reported a traumatic event; 30.5% were exposed to four or more. Five types – witnessing death or serious injury, the unexpected death of a loved one, being mugged, being in a life-threatening automobile accident, and experiencing a life-threatening illness or injury – accounted for over half of all exposures. Exposure varied by country, sociodemographics and history of prior traumatic events. Being married was the most consistent protective factor. Exposure to interpersonal violence had the strongest associations with subsequent traumatic events.
ConclusionsGiven the near ubiquity of exposure, limited resources may best be dedicated to those that are more likely to be further exposed such as victims of interpersonal violence. Identifying mechanisms that account for the associations of prior interpersonal violence with subsequent trauma is critical to develop interventions to prevent revictimization.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Contributors
-
- By Núria Duran Adroher, Sergio Aguilar-Gaxiola, Jordi Alonso, Ali Obaid Al-Hamzawi, Laura Helena Andrade, Matthias C. Angermeyer, James Anthony, Corina Benjet, Guilherme Borges, Joshua Breslau, Evelyn J. Bromet, Ronny Bruffaerts, Brendan Bunting, Huibert Burger, José Miguel Caldas de Almeida, Graça Cardoso, Somnath Chatterji, Wai Tat Chiu, Giovanni de Girolamo, Ron de Graaf, Peter de Jonge, Koen Demyttenaere, John Fayyad, Alize J. Ferrari, Silvia Florescu, Anne M. Gadermann, Meyer Glantz, Jen Green, Michael J. Gruber, Oye Gureje, Josep Maria Haro, Yanling He, Steven G. Heeringa, Hristo Hinkov, Chiyi Hu, Yueqin Huang, Irving Hwang, Robert Jin, Elie G. Karam, Norito Kawakami, Ronald C. Kessler, Lola Kola, Viviane Kovess-Masféty, Michael C. Lane, Carmen Lara, William LeBlanc, Sing Lee, Jean-Pierre Lépine, Daphna Levinson, Zhaorui Liu, Gustavo Loera, Herbert Marschinger, Katie A. McLaughlin, Maria Elena Medina-Mora, Elizabeth Miller, Samuel D. Murphy, Aimee Nasser Karam, Matthew K. Nock, Mark A. Oakley Browne, Siobhan O’Neill, Johan Ormel, Beth-Ellen Pennell, Maria V. Petukhova, José Posada-Villa, Rajesh Sagar, Mohammad Salih Khalaf, Nancy A. Sampson, Kathleen Saunders, Michael Schoenbaum, Kate M. Scott, Soraya Seedat, Victoria Shahly, Dan J. Stein, Hisateru Tachimori, Nezar Ismet Taib, Adley Tsang, T. Bedirhan Üstün, Maria Carmen Viana, Gemma Vilagut, Michael R. Von Korff, J. Elisabeth Wells, Harvey A. Whiteford, David R. Williams, Ben Wu, Miguel Xavier, Alan M. Zaslavsky
- Edited by Jordi Alonso, Universitat Pompeu Fabra, Barcelona, Somnath Chatterji, World Health Organization, Geneva, Yanling He
-
- Book:
- The Burdens of Mental Disorders
- Print publication:
- 09 May 2013, pp ix-xii
-
- Chapter
- Export citation
A pulsar census of the Local Group
- Vladislav Kondratiev, Duncan Lorimer, Maura McLaughlin, Scott Ransom
-
- Journal:
- Proceedings of the International Astronomical Union / Volume 8 / Issue S291 / August 2012
- Published online by Cambridge University Press:
- 20 March 2013, p. 431
- Print publication:
- August 2012
-
- Article
-
- You have access Access
- Export citation
-
We carried out a search for pulsars in nearby galaxies with the GBT and Arecibo radio telescopes at 820 and 327 MHz, correspondingly. Currently, the Magellanic Clouds are the only galaxies except for Milky Way known to harbor radio pulsars, with a total of 20 pulsars being discovered there to date. Discovery of pulsars in other galaxies can be used to trace the history of massive star formation and would allow to probe the intermediate intergalactic medium. We selected 22 galaxies of the Local Group at high galactic latitudes, |b| > 26 deg, with most of them being dwarf spheroidals with old star population. This makes them promising targets to search for giant pulses from recycled millisecond pulsars. Both single-pulse and periodicity searches were performed for trial dispersion measures up to 1000. No extragalactic pulsars are found in half of the selected targets processed so far. I will give the overview of our targetted searches, present potential candidates and discuss the obtained results.
A search for pulsars in the central parsecs of the Galactic center
- Andrew Siemion, Matthew Bailes, Geoff Bower, Jayanth Chennamangalam, Jim Cordes, Paul Demorest, Julia Deneva, Gregory Desvignes, John Ford, Dale Frail, Glenn Jones, Michael Kramer, Joseph Lazio, Duncan Lorimer, Maura McLaughlin, Scott Ransom, Anish Roshi, Mark Wagner, Dan Werthimer, Robert Wharton
-
- Journal:
- Proceedings of the International Astronomical Union / Volume 8 / Issue S291 / August 2012
- Published online by Cambridge University Press:
- 20 March 2013, p. 57
- Print publication:
- August 2012
-
- Article
-
- You have access Access
- Export citation
-
The discovery of a pulsar or pulsars orbiting near the Galactic Center (GC) could offer an unprecedented probe of strong-field gravity, the properties of our galaxy's supermassive black hole and insights into the paradoxical star formation history of the region. However, searching for pulsars near the GC is severely hampered by the large electron densities along our line of sight and the scattering-induced pulse broadening of the pulsar emission observed through it. As the broadened pulse length approaches the pulsar period, the periodicity in pulsar emission becomes nearly undetectable. Searches extended to higher frequencies, in an effort to reduce scattering, suffer from reduced intrinsic flux, higher system temperatures and increased atmospheric opacity. We are currently attempting to mitigate the challenges associated with searching for pulsars near the GC by employing new wide bandwidth receivers, upgraded IF distribution systems and novel digital spectrometers in a GC pulsar search campaign at the Green Bank Telescope in West Virginia, USA.
Our search will cover two frequency bands, from 12-15 GHz (Ku Band) and 18-26 GHz (K Band), during a total of approximately 30 hours of observations, with expected characteristic 10-sigma sensitivities between 5-10 micro-Jy. Our first observations are scheduled for mid-March 2012. Here we will present the status of our observations and initial results.
Childhood maltreatment and DSM-IV adult mental disorders: Comparison of prospective and retrospective findings
- Kate M. Scott, Katie A. McLaughlin, Don A. R. Smith, Pete M. Ellis
-
- Journal:
- The British Journal of Psychiatry / Volume 200 / Issue 6 / June 2012
- Published online by Cambridge University Press:
- 02 January 2018, pp. 469-475
- Print publication:
- June 2012
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
Prior research reports stronger associations between childhood maltreatment and adult psychopathology when maltreatment is assessed retrospectively compared with prospectively, casting doubt on the mental health risk conferred by maltreatment and on the validity of retrospective reports.
AimsTo investigate associations of psychopathology with prospective v. retrospective maltreatment ascertainment.
MethodA nationally representative sample of respondents aged 16–27 years (n = 1413) in New Zealand completed a retrospective assessment of maltreatment and DSM-IV mental disorders. Survey data were linked with a national child protection database to identify respondents with maltreatment records (prospective ascertainment).
ResultsChildhood maltreatment was associated with elevated odds of mood, anxiety and drug disorders (odds ratios = 2.1–4.1), with no difference in association strength between prospective and retrospective groups. Prospectively ascertained maltreatment predicted unfavourable depression course involving early onset, chronicity and impairment.
ConclusionsProspectively and retrospectively assessed maltreatment elevated the risk of psychopathology to a similar degree. Prospectively ascertained maltreatment predicted a more unfavourable depression course.
Comparative migration, growth and development of Typhlocoelum cucumerinum sisowi in dabbling ducks and Typhlocoelum cucumerinum cucumerinum in diving ducks
- Marilyn E. Scott, M. E. Rau, J. D. McLaughlin
-
- Journal:
- Parasitology / Volume 84 / Issue 2 / April 1982
- Published online by Cambridge University Press:
- 06 April 2009, pp. 333-350
-
- Article
- Export citation
-
Experimental infections of mallards (Anas platyrhynchos L.) with Typhlocoelum cucumerinum sisowi (Skrjabin, 1913) and of canvasbacks (Aythya valisineria (Wilson)) with Typhlocoelum cucumerinum cucumerinum (Rudolphi, 1809) revealed significant differences in various parameters of the life-cycle in the definitive host. Both T. c. sisowi and T. c. cucumerinum migrate to the trachea via the abdominal cavity, air sacs and lungs, although T. c. cucumerinum migrate more quickly and more synchronously than T. c. sisowi. Typhlocoelum c. sisowi has a shorter expected life-span than T. c. cucumerinum but grows and reaches maturity more quickly than T. c. cucumerinum. Evidence suggests that T. c. cucumerinum has a higher fecundity than T. c. sisowi. These differences in the patterns of migration, growth and development are related not only to differences between the two host species but also to differences intrinsic to the parasites, and serve to provide biological support for considering them as separate sub-species.







